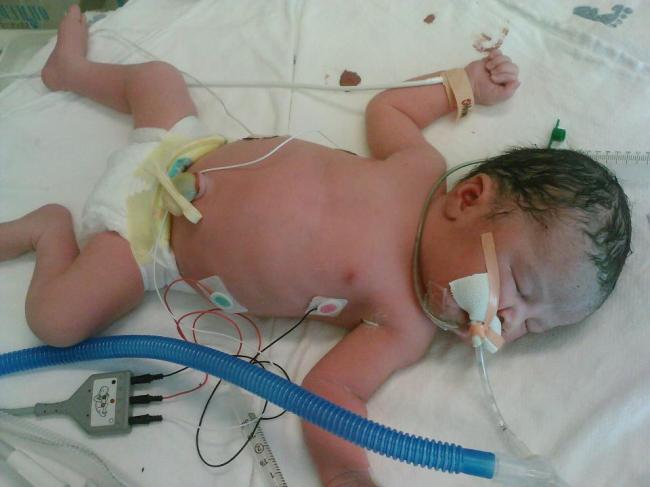
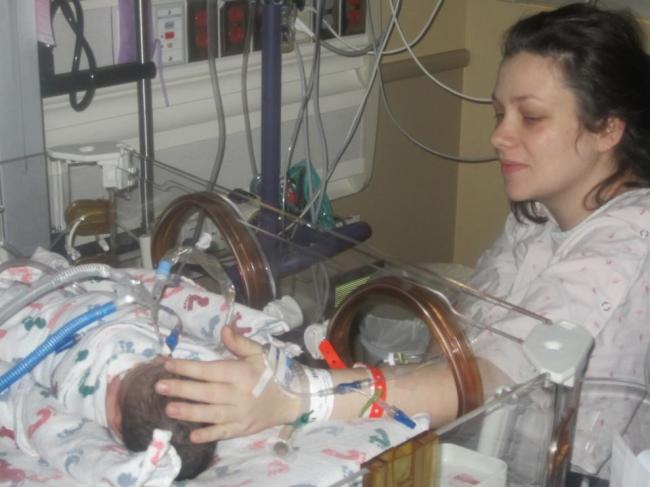
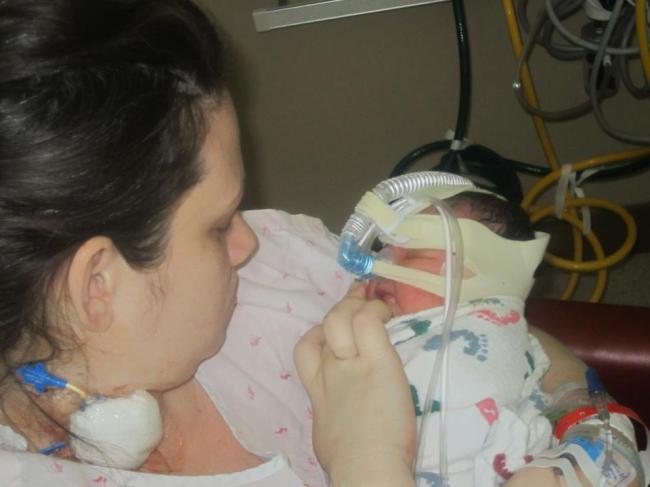
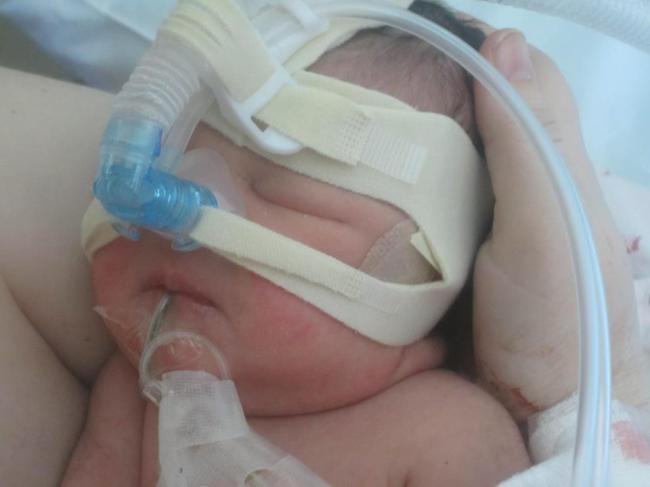
Placenta Previa and Accreta, are life threatening conditions for both Mothers and Babies. While the journey of these pregnancy conditions is stressful and can be heartbreaking, being separated from family and friend, feeling like a like a ticking time bomb, doing what you can in the hope to give your precious baby more time to grow, get strong, and flourish. However there are situations we can't prevent. Labours that can't be stopped, and for many many reasons we can't carry our blessings to term.
These babies are just as much a part of us as all of our others, and we would do what ever we could to have them here and watch them grow. This is a page to honour those babies that didn't make it. If you have lost a baby in the journey of placenta previa, and or placenta accreta, we want to honour that baby. Sharing a photo, picture, name, phrase that speaks to you.
- If you want to add your baby to this post please email me cmathewson.hfa.aus.nz@gmail.com
Sunday, 25 May 2014
Saturday, 24 May 2014
Stephanie's Story with Placenta previa, accreta and AFE
After 7 rounds of intense and emotional IVF
procedures, Stephanie Arnold became pregnant with her second child in October
of 2012. Beginning after her first ultrasound in the 20th week, Stephanie became
overwhelmed with premonitions of her own death. She best explains this feeling
as something that made every cell in her body feel like a ticking time bomb. She
had no idea that what she was feeling would actually come true.
Her daughter Adina was born 2 1/2 years
earlier and delivered by C-Section, so she knew all too well exactly what to
expect during the upcoming birth. Due to a placenta previa diagnosis and
other factors that complicated her pregnancy, she knew that she needed to plan
for the worst. However, it was the premonitions of doom that made planning a
high priority. Rather than accepting bystander status, her husband
Jonathan was able to step into the forefront as a key player to help her. As an
economist, Jonathan realized he needed to set his analytical nature aside and
focus on Stephanie’s worries. He knew that trusting Stephanie’s intuition as
she cried out for someone to listen to her fears and premonitions was critical.
However, in everyone’s defense, there were
no tests or medical books that could have been referenced to predict what was
about to happen. All Stephanie had were the premonitions that had consumed her
entire life. Though, the one difference between previous premonitions and what
she experienced this time around was an overwhelming sense of foreboding. It
was different from the traditional worries everyone experiences from time to
time. The feeling that she would die, including visions of her own death,
penetrated her daily existence and motivated her to get anyone and everyone to
listen.
As her delivery neared, she was fortunate
enough to have one or two people listen to her due to her persistence. She
posted messages on Facebook and even sent goodbye letters. Her feelings were
real so her mission became spreading the message, “If you SENSE something, SAY
something”. And, if no one listens, you say it again, and again and again! She
told everyone that she came into contact with about her premonitions. She hoped
that someone, anyone, would relate to her and give her advice on how to
proceed. But, ultimately, it was left to Stephanie to speak up and avoid
sweeping her feelings under the carpet. Her husband Jonathan was her strongest
ally, supporting her through every appointment and every visit, even if as
Stephanie says, “he thought I was crazy.” It was the love of her husband,
family and friends and all of their support that helped her to become even more
boisterous. After all, she was not ready to leave him permanently or leave her
children motherless.
During her pregnancy, Stephanie surrounded
herself with the best medical professionals and those familiar with what she
was going through. All were convinced and conveyed to her that what she was
afraid of would not happen, and that the probability of it happening was slim
to none. Fortunately, she refused to settle for that and persisted on.
Stephanie assumed people thought she was just hormonal and presumed doctors
thought she was an annoying patient, but it couldn't have been farther from the
truth. Later, she learned that doctors do take premonitions and fear
incredibly seriously. Unfortunately, many patients don’t speak up, so their
doctors never know about their concerns. “They can't read your mind or your
spirit. You know them much better than they ever could and you know yourself
and your needs even better,” says Arnold.
Her own gynecologist, the same doctor that
delivered her daughter Adina, never made her feel like she was crazy. She
understood Stephanie’s fears, but had nothing tangible to work with regarding
her feelings. She supported Stephanie by giving her access to more medical
professionals to speak with. When she opted to go see a gynecology/oncology
specialist, her doctor thought it would be a good idea and was supportive. At
32 weeks she had an MRI which at that point showed no accreta had formed at
that point, and when she asked her doctor how likely would
it be to have an accreta form by the 37th week-- she said, she had never seen
it before. Thinking back, Stephanie believes that her
doctor did not believe what happened to have been possible.
On May30, 2013 Stephanie was 36 weeks and at
home when she suddenly started to hemorrhage. Her husband Jonathan went into
survival mode and rushed her to the hospital for an emergency C-Section. In the
middle of delivering their son Jacob, she coded – flat-lined with all
electrical signs of life gone! Stephanie was clinically dead for 37 seconds and
was kept on life support in a protective coma for 6 days until she stabilized.
Her body was riddled with tubes, ports, and monitoring equipment and she had to
undergo dialysis to rid her body of the edema. However, they saved her life and
brought her back. Today, Stephanie and Jacob suffer no permanent damage, making
them a true medical miracle.
Her ob-gyn, Dr. Julie Levitt, and the
anesthesiologist diagnosed her with placenta accreta and an amniotic fluid embolism (AFE) - a condition where the amniotic fluid enters the mother’s bloodstream,
triggering anaphylactic shock, respiratory failure, cardiac arrest and death.
This occurs when the mother happens to be allergic to the amniotic cells. However,
the condition is very rare, occurring in roughly 1 in 15,200 pregnancies. In
fact, AFE is so rare that Stephanie’s case was the first in the history of
their practice. And, while incidences are low, the condition is the second
leading cause of maternal death in the United States and the United Kingdom.
At 36 weeks she delivered. The amniotic fluid embolism (AFE)
happened and they thought they had the bleed under control when she was put
into SICU. 7 hours later, they realized she was bleeding through the uterus.
Gyn/onc was called in and performed hysterectomy. The pathology showed an
accreta starting to form, which is how the amniotic cells got into the
bloodstream causing the AFE. Not visible to the naked eye, because when
placenta was delivered, it looked complete.
Coming on in two phases, AFE is extremely
catastrophic. In Phase 1, the patient goes into cardiac arrest, the lungs shut
down and the body goes into complete shock. Roughly 40% of patients do not make
it through this phase, however, Stephanie coded here and lived to tell the
tale. Those lucky enough to make it past Phase 1, then have another uphill
battle to fight. The AFE stops the blood’s clotting capability, so many
patients hemorrhage to death. Due to these factors, it’s currently believed
that as many as 85% of AFE patients do not make it out of the operating room. Stephanie
credits her survival to her foresight and the conversations she had with her anesthesiologist
leading up to Jacob’s birth. She requested that they change her anesthesia
order to include more blood, a crash cart and more monitors. “That is 100 percent
what saved my life,” says Arnold.
Stephaine needed 60 units of blood and
blood products which is classes as a massive blood transfusion.
After clinically dying and coming back, Stephanie
has been given a second chance and wants to make every moment count. She
says she has good days and bad days - many times feeling survivors guilt and
wondering why she was chosen to live. Because of this, she makes sure she is
totally present in every second of her life. She values every interaction she
has with others because she believes any day above ground is a good day and she
is more empathetic than ever.
She often reflects back to being in the ICU,
obese with fluid from edema, and recovering from a tragic AFE. The inability to
hold her newborn, let alone spend time with her daughter or her stepdaughter
because she was not coherent is something she will never forget. She has
learned that her family is the most important thing to her and that her husband
will always be there for her. His love and his support got her through
every single day. According to Stephanie, “I was on low voltage with my
intuition because people would look at me like I was a freak if I talked about
things I saw. After losing all electricity in my body, I am now on high voltage
or supercharged and won't allow anyone to make me feel like a freak when I
sense something. Remember, ‘If you SENSE something, SAY something’.” If it will
save a life, it only makes sense to speak up – she knows because it saved hers.
According to Stephanie, “They say it takes
a village and in my case, it did”. Neighbors were there for her and her family. The
Jewish community came together and prayed while other communities also joined
in. One doctor said she couldn't give her a medical reason why she
survived, so she needed to “go spiritual on this one.” And, she was right
as her family leaned heavily on the prayers of the community and its spiritual
leaders.
In her
"previous" life, Stephanie worked for Lubavitch, as a successful
television producer she produced Jewish educational documentaries, including
one about the Rebbe Menachem Schneerson (SP). She is also known for covering the story
rather than being the news, Stephanie’s multi-talented 27 year television
career generated her Emmy Nominations and a Telly-Award as she directed and
produced numerous television series, reality shows, music videos and
documentaries. In her private life she has been a member of Chabad for many
years and was approved to receive a New Hebrew name because of her miraculous
story of death and rebirth. Instead of being recognized by Sarah, she is now
recognized as Chaya Sarah.
For more information about AFE's and the research being done, please
go to www.AFESUPPORT.org for the latest as they are more up to date than your doctors.
Monday, 19 May 2014
World Donor Day - WHO
WHO - World blood donator day, is quickly coming up.
The theme for this year is.............
"Safe blood for Saving mothers"
Many women with Accreta will need a blood transfusion to save their lives, so that they can be here on the other side. The average transfusion for an Accreta mother is 8 units- around 4 litres of blood. Many however will need much more than that. I myself needed 54 Units and 80 blood products from around 134 donations. Without that gift of safe blood I would not be here today to enjoy my baby growing up. WHO Donor day is a time to for us who have received to help give back, by saying a big 'thank you' to all those that have generously given.
If you, like me, have a received the gift of blood donation and want to be a part of giving back to donors this World Blood Donor Day, then send an email: ginawalker@hopeforaccreta.org
"Safe blood for saving mothers"
The focus for this year’s campaign is “Safe blood for saving mothers”. The campaign will increase awareness about why timely access to safe blood and blood products is essential for all countries as part of a comprehensive approach to prevent maternal deaths.
WHO encourages all countries and national and international partners working on blood transfusion and maternal health to develop an activity plan to highlight the need for timely access to safe blood and blood products in the prevention of maternal deaths.

WHO/O. O’Hanlon
Activities may include commemorative events, meetings, publication / dissemination of relevant stories on media outlets, scientific conferences, publication of articles on national, regional and international scientific journals, and other activities that would help in promoting the theme of this year’s World Blood Donor Day (WBDD).
Background information
Every year, on 14 June, countries around the world celebrate World Blood Donor Day. The event raises awareness of the need for safe blood and blood products and to thank voluntary unpaid blood donors for their life-saving gifts of blood.
Every day, about 800 women die from pregnancy or childbirth-related complications. Almost all of these deaths occur in developing countries. More than half of them occur in sub-Saharan Africa and almost one third in South Asia. The risk of maternal mortality is highest for adolescent girls under 15 years of age.
Severe bleeding during delivery and after childbirth is a major cause of mortality, morbidity and long-term disability. However, access to safe and sufficient blood and blood products and the rational and safe use of blood transfusion still remain major challenges in many countries around the world.
The objectives of this year’s global campaign
- Ministries of health, particularly in countries with high rates of maternal mortality, to take concrete steps towards ensuring that health facilities in their countries improve access to safe blood and blood products from volunteer donors for women giving birth.
- National blood services in countries with high rates of maternal mortality to focus on safe blood for mothers in their activities and products for the 2014 campaign.
- Maternal health programmes and partnerships engage in the 2014 campaign.
- WHO and partners throughout the world highlight ." - World Health Organisation
Don't forget if you would like to help, or be a face for the International Hope for Accreta Blood Drive in January 2015, please let us know. We look forward to hearing from you.
- Christina Mathewson
Friday, 16 May 2014
Melissa's Story of Placenta Accreta, Previa, and Hysterectomy
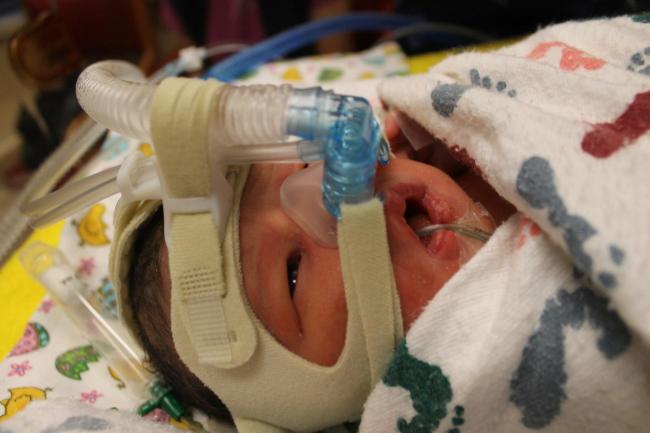
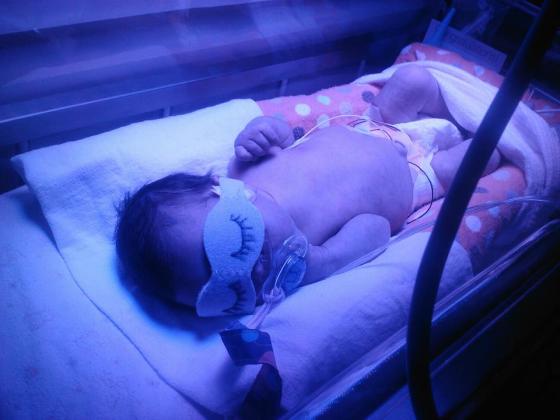
I'm fixated. I'm holding my breath. I'm praying. I'm concentrating intently upon an empty incubator. I have to keep focus upon this plexiglass box towards my right. If I look towards my left I can see a monitor displaying flesh, hands, blood and gore. Those gloved hands, I realise are inside of my body. Those are the hands of the doctors attempting to extract my baby form my uterus. I can't look at that. I focus upon the empty incubator. I continue to pray. I hear a voice ask me, "Melissa. How are you doing?" I look up. It's one of the dozen masked doctors whirling around the room. I look him in the eye and ask, "Is that the baby crying?" He says no. "That is the sound of suction. Your doing great! We're almost there." He walks away. I stare at the empty incubator.
I have been diagnose with placenta previa and placenta accreta. Placenta previa is when your placenta attaches low in your uterus, sometimes covering your cervix. This creates a high risk pregnancy. According to The U.S. National Library of Medicine; "During pregnancy, the placenta moves as the womb stretches and grows. It is very common for the placenta to be low in the womb in early pregnancy. But as the pregnancy continues, the placenta moves to the top of the womb. By the third trimester, the placenta should be near the top of the womb, so the cervix is open for delivery. Sometimes, the placenta partly or completely covers the cervix. This is called a previa. There are different forms of placenta previa. Marginal previa is when the placenta is next to cervix but does not cover the opening. Partial previa is when the placenta covers part of the cervical opening. Or complete previa is when the placenta covers all of the cervical opening."
Having placenta accreta means that your placenta begins to act like an amoeba. It starts to morph and attach to everything around it. It can attach to your uterus, your cervix, and your bladder. When you give birth, it most likely will not detach. So therefore, the doctors have to cut around where the placenta has attached itself. If the placenta has attached to your womb, cervix, they will have to take those along with the placenta. This creates a life threatening situation where you can bleed out, get sepsis, and die if not properly diagnosed and treated.
I remember when I got out of the hospital due to high blood pressure. I was so grateful that I did not have pre-eclampsia. I had pre-eclampsia with my prior children. However; I did have gestational hypertension, gestational diabetes, and now placenta accreta. The doctor said that the best case senerio would be to have a planned cesarean hysterectomy at 36 weeks. The alternative was to risk getting sepsis and possibly dying. I thought, "Thanks Doc. I wonder which door I should to take? Loosing my sex drive and womanhood with a side of crazy or eternal sleep? Decisions. Decisions." I remember being so angry at the doctor. I wondered why the doctor acted like it wasn't a big deal to get a complete hysterectomy. I said to him, "Doctor, sir, I have no desire to have a hysterectomy. I would like to avoid it, if possible." “Oh. You’re not finished having babies? ” “No. Doc. That is not the case. I am definitely finished having babies. But, how would you like to loose 3/4 of your balls? Sure it still works, partially. However; do you still feel like a FULL man?” Of course, I didn't ask that. But I wanted to. I was adamant. I did not want to have a hysterectomy. It's my uterus and I wanted to keep it.
Lying there upon the operating table, I ponder upon my situation. I have both complete placenta previa and placenta accreta. I am an extremely high risk pregnancy. I and my team of doctors had been planning on a C-section, possible hysterectomy on October 11th, 2013. I am 34 weeks pregnant. I am in a room full of doctors, only two of which I know. I am alone with these doctors. My husband was not allowed to be with me in the operating room. I'm in the middle of an emergency c-section. I'm scared. I concentrate upon the incubator.
Looking back, I can not tell this story without including the tale of my other son Sirius. The stress of Sirius' plight caused me to go into preterm labor. Previous to my emergency c-section, it was discovered that our son Sirius was very sick. His illness had begun the week before.Sirius had been walking on his tippy toes and claiming that his ankle hurt. Yet, he still ran around being a his normal jovial toddler self. This was Monday.
- On Tuesday, I took Sirius to daycare, like normal. An hour later, the daycare called me and said that I needed to pick Sirius up. He had not stopped crying and claimed his ankle hurt. I brought him home. My husband and I decided that we would wait to see if his ankle would heal before taking him to the doctor the next day.
- Wednesday, I called his regular doctor. We were unable to make an appointment. So I took Sirius to Urgent care to get x-rays. While there, he started favoring his left ankle & limping on his right. The nurse said he could be faking. After the x-rays came back negative, I began to think the nurse might be right. His diagnosis was a bruised heel. The doctor told me to give him Tylenol and keep him off the ankle as much as possible. He could go back to daycare on Monday.
- Friday night Sirius refused to put any weight on his left foot. He started crawling like a baby around the house. He came down with a fever. Now I want to note that there was so swelling of the ankle. And Sirius was still wanting to play and go outside. But I knew something was wrong. I just didn't know how serious I should take it.
- Saturday and Sunday I went back and forth between Tylenol and Motrin to keep his fever down. It never went away, just went down a few degrees. He seemed to progressively get worse. I didn't want to take him back to Urgent Care. On Monday Sept. 23rd, I was able to get him into his regular doctor.
That morning, I had an OB appointment. My husband Scott took Sirius to the doctor. While there, they took x-rays again. They came back negative. The doctor ordered labs. That's when the roller coaster ride began. Sirius' white blood cell count was off the charts, the doctor explained.We needed to take our son to the emergency room immediately. I had a morning appointment at OU Children's Hospital the next day. So, I figured that would be the best place to go in case he had to stay overnight.
My little family waited in the big waiting room. You normally have to wait awhile in the emergency room before being seen. Not this time. Not for us. In a short time we were called into a smaller waiting room. There we met an Orthopedic surgeon that told us that Sirius had what was known as septic joint. He had to be operated upon immediately. The surgeon was explaining Sirius' diagnosis and the eminent surgery. I saw the man's lips moving. I barely could comprehend what he was saying. How could this be happening? My poor baby! It's my fault. I heard the words blood infection, sepsis, and critical condition. All of the sudden, I felt a large gush. I looked down to realize that blood was all over the chair and the floor.
Everything seemed to slow down in that moment. I evaluated my situation. Where am I? I'm in the hospital. Why am I here? Because my son is sick. What am I to do? Deal with it. I began to cry. My daughter started crying. My husband was reserved. My son was sick and sucking his thumb, asleep in his stroller. They brought me a wheelchair and carted me off to maternity urgent care.
While there, my hemorrhaging became increasingly worse. They began to prep me for an emergency c-section. The panic that I felt accelerated to a screaming roar. I couldn't have my baby now, I pleaded. My husband could not be with me. My husband had to be with my son during his operation. He was being prepped at that moment! I want to be with my son! He needs me. How could this happen?! What bad timing!
I soon endured hours of torture that entailed, but was not limited to; magnesium sulfate drip, starvation and denial of water. I was poked and prodded for IV lines. And the most fun of all, I was subjected to a catheter.The doctor came to tell me that they were going to move me out of Urgent Care. I was moved to a new room on the maternity floor. There, I waited for hours to find out if I was to have an emergency c-section. I hoped that they would put me on hospital bed rest. I prayed that they would let me wait to have the baby on my scheduled c-section, three weeks away. My hopes were dashed when the doctor came in to tell me that they had scheduled my c-section at 11:00 the next morning. No ands, ifs, or buts about it. And I needed to prepare myself for a possible hysterectomy. Fabulous.
I called my husband for an update on our son. It had been decided that the doctors would post pone his operation until 11:00 the next morning. The exact same time that I was to give birth. They had given Sirius morphine for the pain, and he was asleep for the time being. Morphine. My three year old son needed a full blown morphine drip for his pain. I had been giving him Tylenol & Motrin and thinking he might have been faking. I officially felt like an asshole. I couldn't even be there to comfort him.
It occurred to me that this situation was way beyond my control. My only options were to leave the situation to God, pray, and focus upon the task at hand.
On September 24th, 2013 at 1:13 PM, my son Corvus Asher Clark came into this world blue and not breathing. I remember, it took five minutes for my third child to take his first breath. I heard him cry like a kitten. He was quickly presented to me so I would be able to see his little face. I kissed him. I watched the doctors place my baby into the incubator. I finally could breathe. Corvus Asher was whisked away in the incubator and delivered to the neonatal intensive care unit. He was 34 weeks plus 3 days gestational age. He weighed 5lbs 3 ozs and was 17 inches long.
Immediately, the doctors attempted to detach my placenta from my uterus and cervix. It seemed as if it was going to come off cleanly. Alas, it did not. My complete placenta previa / accreta would not allow it to happen. They told me that it was time now to go to sleep. And that's what I did. I slept for another 5 hours while they carved my placenta, uterus, and cervix from my body.
My son Sirius had to have a total of three operations on his left tibia to flush out the infection. He had what is known as MRSA. MRSA is an antibiotic resistant staff infection. Very heinous stuff. He was in the hospital for a total of three and a half weeks. They released him with a PICC line. He sported that for and additional eight weeks. By the grace of the Lord, he's healthy now. You can't even tell he was ever sick.
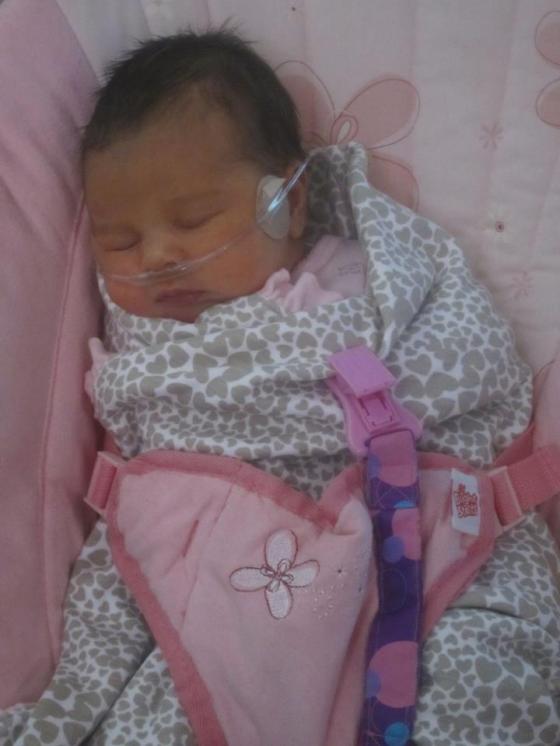
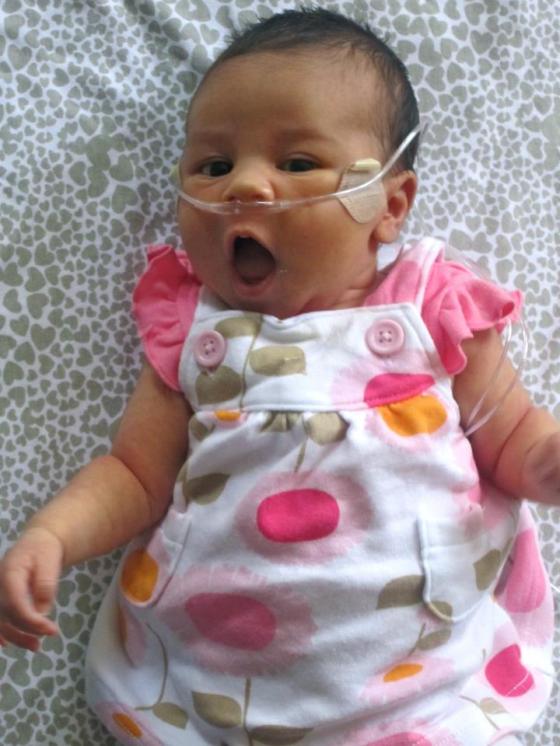
Corvus Asher had to wear a cpap to help him breathe for three days. He had jaundice. He had to stay in NICU for 13 days total. Even though he was preterm, and he did not breathe for the first five minutes of his life, there is absolutely nothing wrong with him. He is as perfect as any baby could be.
I was released from the hospital first, out of the three of us, after six days. I did not have time to nurture myself and heal. I ran on overdrive. I had two boys in the hospital, at the same time. I had a daughter and husband to care for. I had to put all my focus upon their healing. And they did heal. I healed too. Other than a nasty vertical scar that goes from my belly button towards my nether region, and having to have two pints of blood transfusion, I feel absolutely no damage from the experience.
Pertaining to my uterus, it's strange knowing that part of your body is dead. Never to be alive again. I thought that it might have been a decent gesture to give my dead uterus back to me. I could've built a little cedar coffin so that I may bury it in my back yard. Do a service over it. Plant a tree, possibly. Is that's too macabre? Maybe. But it's too late. My uterus is gone forever. I wonder what they did with it. Did they burn it? Did it go over to the college for the medical students to study? Did they trash it? My poor wrecked uterus sitting at the bottom of a trash can. I shudder to think of it.
I'm OK with not having a uterus. My son is alive. Both my sons are alive. For this, I am truly grateful. Asher is quite the consolation prize. The whole experience feels strangely surreal. But I don't morn my uterus being gone as much as I thought I would. I was afraid that having a hysterectomy would kill my love life. Thank goodness, that did not come to fruition. I will never have a period again. Who wants a monthly bloody mess anyway? I will never be able to be fertile again. I have three children. When my youngest is 18, I will be 55. It's OK. I'm done having babies. I accept it.
So, what is to be learned from this experience? I guess the main thing that I learned was when everything is absolutely crazy, you have no control over the situation, it is the utmost importance to have faith. You must give your troubles to your higher power and pray, breathe, and keep focused upon the task at hand. If you do that, things should work out the way that they are meant to be. Even if that means you must loose an organ in the process. Life will carry on.
Sunday, 4 May 2014
Stephanie and Anne's Story - Accreta
Wednesday, May 2, 2012 began much like any other day. It was two days before I was scheduled to have Annie via c-section. The weekend before I had been in Labor and Delivery due to some spotting, and was sent home with instructions to rest. Just as my husband was leaving for work that Wednesday morning, I discovered I was spotting yet again, this time passing large clots of blood. I told Tristan not to leave for work until I spoke to the doctor’s office. I called and sure enough, I was told to head to L&D again. I was assuming that I would be checked, cleared, and sent home to wait another two days for my scheduled c-section/hysterectomy, so the husband and I packed up the three kids in the van and headed to the hospital. I got settled into a little triage room in L&D, and Tristan took the girls to the hospital cafeteria for some breakfast. Because of the complications with my pregnancy, I was seeing the high risk obstetrics group based out of the hospital, so one of the midwives came in to see me right away. She checked me and asked some questions about my visit to the hospital the previous weekend. She said I was definitely bleeding, then she left the room. She came back in with a nurse a few minutes later, and I noticed right away that the nurse was dressed for surgery. I assumed that she must be getting ready to head to some c-section, because no one had said anything to me. I was hooked up to some monitors, then they left the room again. A few minutes later, someone came in to take blood for some blood work. While that person was in, the nurse returned along with the midwife, and then more people came in. It was a tiny little triage room, but it was suddenly filled with people doing paperwork and asking me questions. Finally, I spoke up and said, “Can someone please tell me what is going on here?” The midwife looked at me and said, “Honey, you’re having a baby today.” I was stunned! She said, “No one told you?” All I could do was laugh. Would I have been so shocked if I knew I was about to have a baby?? My next question was “Why?” immediately followed by, “When?” It seemed that with all the problems going on in my uterus, and this being the second time in a matter of days that I was seen for bleeding, they were concerned that my uterus and placenta weren’t going to hold out for another two days, so they made the decision to deliver that morning. I would be headed to the OR within the hour! I pulled out my cell phone and called Tristan, who had just settled the girls down at a table in the cafeteria to feed them. I said, “We’re having a baby today!” So, he called his parents to come pick up the kids, and then loaded the younger two into the double stroller and they all headed back up to Labor and Delivery. It’s hard to remember all the details at this point, because everything started happening so fast. People were coming and going from that little triage room. I was signing papers, answering questions, and trying hard to comprehend what was happening. They put two humongous IVs in each hand. They said with the major surgery I was about to have, that they needed at least two IVs in for all the various things I may need, like medications and blood transfusions. I recall that it took them several times to get the IV in to my right hand, and there was blood all over the blanket. I asked them to please hide the blood, because I didn’t want to scare my 6 year old when she came up to see me before the surgery. My husband and children came into the room, but they couldn’t stay long because the room was crammed full of nurses, midwives and doctors coming and going. I recall that our pastor came in at one point and prayed, and then I was taken to the pre-op area. I nearly cried as they wheeled me down the hall and away from my husband and daughters. It all happened so fast that I had absolutely no time to process anything!
The next thing I remember is being taken a very long way to the OR. Because of the nature of my surgery, it was not to be done in the L&D operating room, where they typically do c-sections. This surgery was to be done in the main OR, on the other side of the hospital. At the pre-op area I was one again met by the sweet midwife. She talked to me a lot, but I don’t remember anything she said. Several doctors came and introduced themselves. There was the anesthesiologist, a urologist, a vascular surgeon, and I’m not sure who else. The whole time this was happening, I recall that Annie was very active in my belly. I was flat on my back on the gurney, so I was able to see all the kicks and rolls as the baby made her presence known. I remember thinking, “Have fun now, Baby, because you have no idea what’s in store for you in a few minutes!” Then I was wheeled into the OR. The nurses helped me roll from the gurney onto the operating table. Those tables are so uncomfortable. You are literally lying on a board, flat on your back. Let me tell you, that is NOT the most comfortable position to be in when your are hugely pregnant. They stretched out each arm and strapped them down, then placed straps around my chest and belly. I remember looking around the room and being absolutely amazed at just how many people there were! There were countless doctors, nurses, surgical techs, and an entire team from the NICU waiting on the baby. This was not my first surgery, nor was it my first c-section, but I had never seen so many people in one operating room! The anesthesiologist came in and sat down by my head. He explained that he would be giving me some medication to relax me, and then once I was asleep he would be placing a central line in my neck. An oxygen mask was placed on my face and I was told to take deep breaths. I was scared, and tears began to fall. And then I slept.
The next thing I knew, I was being woken up in recovery. I don’t know how it is possible, but it felt as if a very, very long time had passed since I was in that OR. It should have seemed quick, but it didn’t. It felt like I had been asleep for hours and hours. Days, even. There were lots of voices calling my name, talking to me, asking questions, but all I knew was pain. There are no words to properly describe the pain I was in. My insides were on fire, being twisted into knots, and cut into pieces all at once. All I could do was cry. A nurse was telling me to hold on, that they were getting pain medication into my IV. The anesthesiologist came and gave me something, but no relief came. He tried something else, and still something more, but the pain continued. I thought I was going to die from that pain. Finally, he said I could have an epidural, but I was warned that I would have to sit up and bend over for it. I was willing to do anything to make that pain stop. I sat up, and I nearly blacked out from the pain. Two nurses helped me to stay in the position for the epidural. It was placed, and the relief came over me so quickly, I hardly knew what to do with myself! I was placed back into the bed, and finally I could think and talk and comprehend. I asked what had happened, and why I was in so much pain. They explained that I had hemorrhaged during the surgery, and lost about a third of my blood. I was given Pitocin to make my uterus contract to stop the hemorrhaging. I realized as I was being told this that I must still have a uterus. What a surprise that was, because I went into the surgery expecting a hysterectomy! It seems that my placenta was only attached to my uterus in one area, about the side of a half dollar. They were able to remove that section of my uterus and sew it shut, and spare removing the entire uterus. This was a blessing. Because of scarring from previous c-sections, I have a lot of adhesions. Basically, my bladder is permanently stuck to my uterus, and my uterus is permanently attached to the inside of my abdominal wall. They wanted to avoid a full hysterectomy if they could because of the amount of vascular damage that would have been done to remove it, as well as having to remove part of my bladder. God was good, and they only needed to remove a section my my uterus. This brings me back to the pain I was in. You see, not only was a portion of my uterus removed and the hole sewn shut, but the uterus had also been cut open to remove the baby and placenta, which was a huge incision that opened my abdomen from top to bottom, and then sewn shut. On top of that, I was given Pitocin to make that same uterus have contractions after being cut into in several different places. They hadn’t given me any pain medication prior to waking me, because they wanted to judge my pain level and medicate accordingly. So there I was, wide awake and feeling every single ounce of pain as my poor, patched-up uterus was contracting, and then I was made to sit up and curl into a ball at the edge of the bed while they gave me the epidural. At this point I was no longer in pain, so I could actually laugh about the fact that I got my first ever epidural AFTER giving birth.
I asked several times about the baby, but no one knew. They kept telling me that they would call over to the NICU for an update, but that she was probably doing fine. They were able to give me her stats: she was 6 lbs 4 oz and 19 3/4 inches long. My smallest, but longest baby yet! Not bad for a 36 weeker.
I was taken from the recovery room to the ICU for monitoring. Tristan came in soon after and gave me news about the baby. They felt like she was doing well – considering what she had been through – but she was intubated because she wasn’t able to breathe on her own. I didn’t understand how they could be so optimistic while my baby was on a ventilator! He snapped some photos with my camera and I was able to finally see her for the first time on that tiny little screen. The sight just about broke my heart. There was my tiny little baby with a breathing tube down her mouth, an IV in her, and spots of blood on the blanket she was lying on. All I could do was cry. I needed to know what was happening and why. One of the doctors who performed my surgery came in and spoke to me, and explained a little about what happened. It seems that I was under anesthesia for the better part of an hour before they finally got the baby out. There were unforeseen complications that arose as they placed the stents in my ureters before operating, and then as they began to operate, that slowed things down significantly. Also, they wanted to take their time so as not to cause any potential damage to my placenta, ureters, and other parts. When they finally got Annie out, she had been exposed to the anesthesia for a long time herself, and was so sedated that she was unable to breathe on her own. Fortunately they had the full NICU team and neonatologist on hand in the OR, and they were able to act immediately and rush her straight to the NICU. But everyone kept saying she was doing well, and that she would be off the vent and perfectly fine by the next day. I visited with Tristan for a little while, but I was anxious that someone should be with the baby at all times, so I sent him back to the NICU to be with her.
A little while later, the nurse came in to check on me. She had me try sitting at the edge of the bed to see how I would do. As I sat there, I had a very strange sensation like something was dripping down my back. She assured me it was just normal sensations from the epidural, and helped me to lie back down in the bed. Within minutes, my pain came back. I was in tears again. I paged the nurse, and she called the anesthesiologist. The epidural was turned up, but it barely took the edge off the pain. I was having a really hard time managing it. Finally, the anesthesiologist came in and checked the epidural. Apparently it came out when the nurse had me sit up, and most of the medication was leaking out (hence the dripping sensation I felt when I was sitting up). I was only getting enough medication to take the edge off. At that point the anesthesiologist decided to switch me over to an IV medication pump. I got pain meds through the IV, and there was a little pump that allowed me to get an extra little boost in medication every so often by pressing a button. As long as I stayed on top of pressing that button, I was able to mostly manage the pain. I stayed in the room being monitored and feeling like I was going to lose my mind for hours. I couldn’t sleep because I was too busy trying to keep the pain under control. Tristan came and went several times, going back and forth between the NICU and the ICU. Nothing was changing with Annie, and it was looking less and less likely that she was going to bounce back like they initially has said.
Finally, at around midnight I was told that I could go see her. I was helped into a wheelchair and taken to the NICU. That sight will never leave me, as long as I live. There was my tiny little angel, sleeping in the incubator with all kinds of things hooked to her. She didn’t even stir when I touched her and spoke to her because she was still so sedated. I couldn’t hold her, but I got to touch her and stroke her precious little head. I stayed as long as I could, but the pain was picking up again and I had to get back to my room. I was finally able to sleep a little after getting to see my baby.
Later that morning I was moved to the maternity ward because I was recovering well. It was not easy to be there and see all the moms with their babies, while my baby was over in the NICU and separated from me. I pumped every 2 hours to try and get my milk to come in as soon as possible, although they weren’t allowing her to eat at this point. They saved what I pumped though, and would give it to her via the OG tube once the doctor allowed her to begin eating. At this point, she was receiving what she needed from the IV. Later that day I was given the happy news that she was being taken off the ventilator and moved to a CPAP, which was a step in the right direction. I was also told that I would be able to hold her once that happened. I pestered the nurses and NICU staff constantly, and as soon as I got the news that she was switched to the CPAP, they wheeled me back to the NICU so I could hold her. Oh, what a wonderful thing that was! I still couldn’t nurse her, but it was wonderful to have my baby in my arms and be able to have some skin-to-skin time. I even got to see her with her eyes open for a moment!
She still slept most of the time, though. I visited her every few hours, and pumped in between. I slept very little, but I was okay because all I cared about was devoting every waking second to getting my baby better. I was weak and exhausted, but I assumed it was because of the lack of sleep. Everyone kept telling me how pale I was, and I was having some breathing difficulties, but I was completely distracted by the baby’s needs. I was still struggling to manage the pain, but I was forcing myself to get up and walk and speed up my recovery for Annie’s sake.
At this point bad news seemed to come every time I got an update. Annie’s lungs were filled with fluid so her breathing was labored. They suspected pneumonia and ordered tests. Blood work came back showing an infection. It went from her being expected to be released from the NICU in 24 hours to being told she would probably be there for at least a month. She had done a little better and they were lowering her oxygen level, but then she regressed and they needed to increase her oxygen. They cultured mucous samples from her lungs because of the blood work indicating an infection. At one point they tried to get an IV in through her umbilical cord, but the IV broke off inside her. That happened while Tristan I were in the room with her. They kicked us out of the room and paged the neonatologist. They were just about to rush her into surgery when the doctor managed to get it out. It seemed like every time I turned around, I was being terrorized with more bad news.
On day three she was moved from the CPAP to a high flow nasal cannula. This was what I had been waiting for – I could finally nurse my baby! Up to that point she had been given what I pumped mixed with a little donor milk and fed through her OG tube (a tiny tube run down her mouth into her stomach). I was very happy that she took right to breastfeeding and we had no issues getting her to latch! She was weighed before and after each feed to see how much she got. My milk still wasn’t in yet, but she was getting colostrum. The would then supplement the rest if her feed with donor milk through the tube with was now fed down her nose and into her stomach. I nursed her every three hours on the dot. I would set an alarm on my cell phone and when it went off, I would head down the long hall from the maternity ward to the NICU. I would go through the cycle of washing my hands in the wash area, then head to her “pod” (which was what they called her little room). I would change her diaper, then nurse her, then put her back into the bed and head back to my room. Then I would pump so I could get my milk to come in. After that I would sleep for about an hour, then get up and do it again.
I was still so exhausted and pale. I was on oxygen now, and every time they tried to take me off my oxygen levels would drop. My doctor was concerned. She ordered some blood tests, and it seems that the blood I lost during surgery was not replenishing on its own, so she ordered a transfusion. I wasn’t exactly happy about that, but after I got it I became to feel so much better! My color began to return, and I started to feel better within hours. My pain was under control at this point, and my recovery was coming along. Annie was also beginning to do well, for which I was so grateful. They were able to rule out an infection. It seems the blood work they initially did was somehow tainted, and the mucus sample showed no infection. She was breathing a little better every day.
Then we had another setback. She developed jaundice and her bilirubin levels got too high. She had to be under the bill lights to get her levels down. We were told that as soon as she began to gain some weight and get her bilirubin levels stabilized, she could go home, but that she would have to be on home oxygen for an unknown amount of time.
On day four my milk came in. I was thrilled! She no longer needed any supplementary donor milk, so the NG tube was removed. She was also moved to a low flow nasal cannula at this point, but her bilirubin was still too high. I continued the routine of nursing every three hours, always going back and forth between the NICU and my room in the mother/baby wing. My life revolved around that tiny little baby, and I was beginning to forget what like was like outside the NICU! I slept very little, but I welcomed the exhaustion. On day six I was discharged from the hospital. I packed up all my stuff and headed straight to Annie’s room. I was prepared to sleep in the little chair by her bed until she was also discharged from the hospital, but a miracle occurred! Over night she put on weight and her bilirubin numbers decreased. They told me that I could room-in with her in a special room that they had in the NICU for babies who were about to be released. That night was the first time that I was able to be with my baby all night long. I slept in the bed, and her little bassinet was right there by my side.
The next morning they did more blood work and weighed her again. She passed with flying colors, so we were given the okay to bring her home. How thankful I was!! It felt wonderful to finally be at home with all four of my children.
She was sent him on oxygen and we had to have a big tank in the house, plus little travel oxygen tanks for when we went out. It took some getting used to, but it was worth it to have her at home with us, and thankfully she only needed it for a month.
It took some time for me to come to terms with everything. Things were so hectic at the hospital that I never had the chance to process anything that happened. When I got home, I immediately began having nightmares about horrible things happening to my baby at the hospital, or bad things happening to me during surgery. That went on for weeks and weeks, and I struggled to sleep because of it. I would lay awake for hours, replaying everything that happened and remembering the fear of not knowing what was going to happen to my baby, and when I did sleep I was terrorized by nightmares. But, slowly, I began to move away from the pain. I am thankful that right aroud this time we got the news that we were going to be relocating because of my husband’s job, as it was able to consume my thoughts and help me emotionally recover from everything that happened during that week at the hospital. I am truly grateful for the care we received at the hospital. I’m thankful for the donor breastmilk that helped my baby before my milk came in, and for the surgery and blood transfusions that saved my life. I am thankful for God’s hand, that was so clearly there every step of the way.
It’s been nearly two years since Annie was born, and she is still every bit the miracle that she was then. She is happy, healthy, and she completes our family perfectly. I am also happy to report that she is still breastfeeding like a champ! Not a day goes by that I don’t give thanks to the Lord for this precious gift he’s given us.
Subscribe to:
Posts (Atom)