Wednesday, May 2, 2012 began much like any other day. It was two days before I was scheduled to have Annie via c-section. The weekend before I had been in Labor and Delivery due to some spotting, and was sent home with instructions to rest. Just as my husband was leaving for work that Wednesday morning, I discovered I was spotting yet again, this time passing large clots of blood. I told Tristan not to leave for work until I spoke to the doctor’s office. I called and sure enough, I was told to head to L&D again. I was assuming that I would be checked, cleared, and sent home to wait another two days for my scheduled c-section/hysterectomy, so the husband and I packed up the three kids in the van and headed to the hospital. I got settled into a little triage room in L&D, and Tristan took the girls to the hospital cafeteria for some breakfast. Because of the complications with my pregnancy, I was seeing the high risk obstetrics group based out of the hospital, so one of the midwives came in to see me right away. She checked me and asked some questions about my visit to the hospital the previous weekend. She said I was definitely bleeding, then she left the room. She came back in with a nurse a few minutes later, and I noticed right away that the nurse was dressed for surgery. I assumed that she must be getting ready to head to some c-section, because no one had said anything to me. I was hooked up to some monitors, then they left the room again. A few minutes later, someone came in to take blood for some blood work. While that person was in, the nurse returned along with the midwife, and then more people came in. It was a tiny little triage room, but it was suddenly filled with people doing paperwork and asking me questions. Finally, I spoke up and said, “Can someone please tell me what is going on here?” The midwife looked at me and said, “Honey, you’re having a baby today.” I was stunned! She said, “No one told you?” All I could do was laugh. Would I have been so shocked if I knew I was about to have a baby?? My next question was “Why?” immediately followed by, “When?” It seemed that with all the problems going on in my uterus, and this being the second time in a matter of days that I was seen for bleeding, they were concerned that my uterus and placenta weren’t going to hold out for another two days, so they made the decision to deliver that morning. I would be headed to the OR within the hour! I pulled out my cell phone and called Tristan, who had just settled the girls down at a table in the cafeteria to feed them. I said, “We’re having a baby today!” So, he called his parents to come pick up the kids, and then loaded the younger two into the double stroller and they all headed back up to Labor and Delivery. It’s hard to remember all the details at this point, because everything started happening so fast. People were coming and going from that little triage room. I was signing papers, answering questions, and trying hard to comprehend what was happening. They put two humongous IVs in each hand. They said with the major surgery I was about to have, that they needed at least two IVs in for all the various things I may need, like medications and blood transfusions. I recall that it took them several times to get the IV in to my right hand, and there was blood all over the blanket. I asked them to please hide the blood, because I didn’t want to scare my 6 year old when she came up to see me before the surgery. My husband and children came into the room, but they couldn’t stay long because the room was crammed full of nurses, midwives and doctors coming and going. I recall that our pastor came in at one point and prayed, and then I was taken to the pre-op area. I nearly cried as they wheeled me down the hall and away from my husband and daughters. It all happened so fast that I had absolutely no time to process anything!
The next thing I remember is being taken a very long way to the OR. Because of the nature of my surgery, it was not to be done in the L&D operating room, where they typically do c-sections. This surgery was to be done in the main OR, on the other side of the hospital. At the pre-op area I was one again met by the sweet midwife. She talked to me a lot, but I don’t remember anything she said. Several doctors came and introduced themselves. There was the anesthesiologist, a urologist, a vascular surgeon, and I’m not sure who else. The whole time this was happening, I recall that Annie was very active in my belly. I was flat on my back on the gurney, so I was able to see all the kicks and rolls as the baby made her presence known. I remember thinking, “Have fun now, Baby, because you have no idea what’s in store for you in a few minutes!” Then I was wheeled into the OR. The nurses helped me roll from the gurney onto the operating table. Those tables are so uncomfortable. You are literally lying on a board, flat on your back. Let me tell you, that is NOT the most comfortable position to be in when your are hugely pregnant. They stretched out each arm and strapped them down, then placed straps around my chest and belly. I remember looking around the room and being absolutely amazed at just how many people there were! There were countless doctors, nurses, surgical techs, and an entire team from the NICU waiting on the baby. This was not my first surgery, nor was it my first c-section, but I had never seen so many people in one operating room! The anesthesiologist came in and sat down by my head. He explained that he would be giving me some medication to relax me, and then once I was asleep he would be placing a central line in my neck. An oxygen mask was placed on my face and I was told to take deep breaths. I was scared, and tears began to fall. And then I slept.
The next thing I knew, I was being woken up in recovery. I don’t know how it is possible, but it felt as if a very, very long time had passed since I was in that OR. It should have seemed quick, but it didn’t. It felt like I had been asleep for hours and hours. Days, even. There were lots of voices calling my name, talking to me, asking questions, but all I knew was pain. There are no words to properly describe the pain I was in. My insides were on fire, being twisted into knots, and cut into pieces all at once. All I could do was cry. A nurse was telling me to hold on, that they were getting pain medication into my IV. The anesthesiologist came and gave me something, but no relief came. He tried something else, and still something more, but the pain continued. I thought I was going to die from that pain. Finally, he said I could have an epidural, but I was warned that I would have to sit up and bend over for it. I was willing to do anything to make that pain stop. I sat up, and I nearly blacked out from the pain. Two nurses helped me to stay in the position for the epidural. It was placed, and the relief came over me so quickly, I hardly knew what to do with myself! I was placed back into the bed, and finally I could think and talk and comprehend. I asked what had happened, and why I was in so much pain. They explained that I had hemorrhaged during the surgery, and lost about a third of my blood. I was given Pitocin to make my uterus contract to stop the hemorrhaging. I realized as I was being told this that I must still have a uterus. What a surprise that was, because I went into the surgery expecting a hysterectomy! It seems that my placenta was only attached to my uterus in one area, about the side of a half dollar. They were able to remove that section of my uterus and sew it shut, and spare removing the entire uterus. This was a blessing. Because of scarring from previous c-sections, I have a lot of adhesions. Basically, my bladder is permanently stuck to my uterus, and my uterus is permanently attached to the inside of my abdominal wall. They wanted to avoid a full hysterectomy if they could because of the amount of vascular damage that would have been done to remove it, as well as having to remove part of my bladder. God was good, and they only needed to remove a section my my uterus. This brings me back to the pain I was in. You see, not only was a portion of my uterus removed and the hole sewn shut, but the uterus had also been cut open to remove the baby and placenta, which was a huge incision that opened my abdomen from top to bottom, and then sewn shut. On top of that, I was given Pitocin to make that same uterus have contractions after being cut into in several different places. They hadn’t given me any pain medication prior to waking me, because they wanted to judge my pain level and medicate accordingly. So there I was, wide awake and feeling every single ounce of pain as my poor, patched-up uterus was contracting, and then I was made to sit up and curl into a ball at the edge of the bed while they gave me the epidural. At this point I was no longer in pain, so I could actually laugh about the fact that I got my first ever epidural AFTER giving birth.
I asked several times about the baby, but no one knew. They kept telling me that they would call over to the NICU for an update, but that she was probably doing fine. They were able to give me her stats: she was 6 lbs 4 oz and 19 3/4 inches long. My smallest, but longest baby yet! Not bad for a 36 weeker.
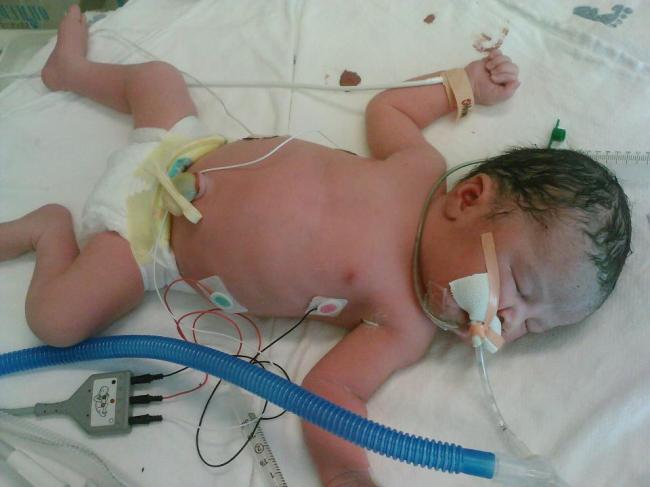
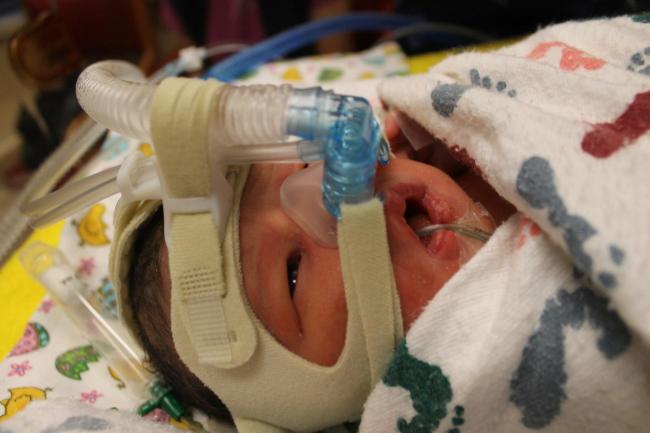
I was taken from the recovery room to the ICU for monitoring. Tristan came in soon after and gave me news about the baby. They felt like she was doing well – considering what she had been through – but she was intubated because she wasn’t able to breathe on her own. I didn’t understand how they could be so optimistic while my baby was on a ventilator! He snapped some photos with my camera and I was able to finally see her for the first time on that tiny little screen. The sight just about broke my heart. There was my tiny little baby with a breathing tube down her mouth, an IV in her, and spots of blood on the blanket she was lying on. All I could do was cry. I needed to know what was happening and why. One of the doctors who performed my surgery came in and spoke to me, and explained a little about what happened. It seems that I was under anesthesia for the better part of an hour before they finally got the baby out. There were unforeseen complications that arose as they placed the stents in my ureters before operating, and then as they began to operate, that slowed things down significantly. Also, they wanted to take their time so as not to cause any potential damage to my placenta, ureters, and other parts. When they finally got Annie out, she had been exposed to the anesthesia for a long time herself, and was so sedated that she was unable to breathe on her own. Fortunately they had the full NICU team and neonatologist on hand in the OR, and they were able to act immediately and rush her straight to the NICU. But everyone kept saying she was doing well, and that she would be off the vent and perfectly fine by the next day. I visited with Tristan for a little while, but I was anxious that someone should be with the baby at all times, so I sent him back to the NICU to be with her.
A little while later, the nurse came in to check on me. She had me try sitting at the edge of the bed to see how I would do. As I sat there, I had a very strange sensation like something was dripping down my back. She assured me it was just normal sensations from the epidural, and helped me to lie back down in the bed. Within minutes, my pain came back. I was in tears again. I paged the nurse, and she called the anesthesiologist. The epidural was turned up, but it barely took the edge off the pain. I was having a really hard time managing it. Finally, the anesthesiologist came in and checked the epidural. Apparently it came out when the nurse had me sit up, and most of the medication was leaking out (hence the dripping sensation I felt when I was sitting up). I was only getting enough medication to take the edge off. At that point the anesthesiologist decided to switch me over to an IV medication pump. I got pain meds through the IV, and there was a little pump that allowed me to get an extra little boost in medication every so often by pressing a button. As long as I stayed on top of pressing that button, I was able to mostly manage the pain. I stayed in the room being monitored and feeling like I was going to lose my mind for hours. I couldn’t sleep because I was too busy trying to keep the pain under control. Tristan came and went several times, going back and forth between the NICU and the ICU. Nothing was changing with Annie, and it was looking less and less likely that she was going to bounce back like they initially has said.
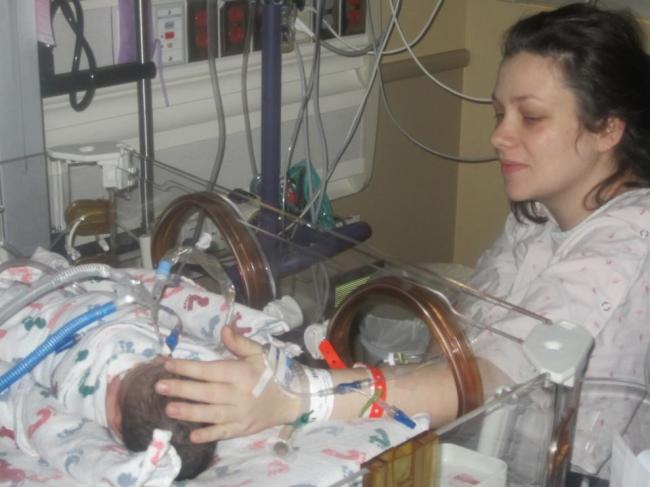
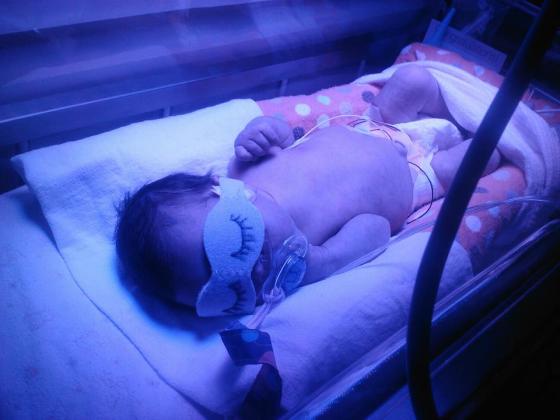
Finally, at around midnight I was told that I could go see her. I was helped into a wheelchair and taken to the NICU. That sight will never leave me, as long as I live. There was my tiny little angel, sleeping in the incubator with all kinds of things hooked to her. She didn’t even stir when I touched her and spoke to her because she was still so sedated. I couldn’t hold her, but I got to touch her and stroke her precious little head. I stayed as long as I could, but the pain was picking up again and I had to get back to my room. I was finally able to sleep a little after getting to see my baby.
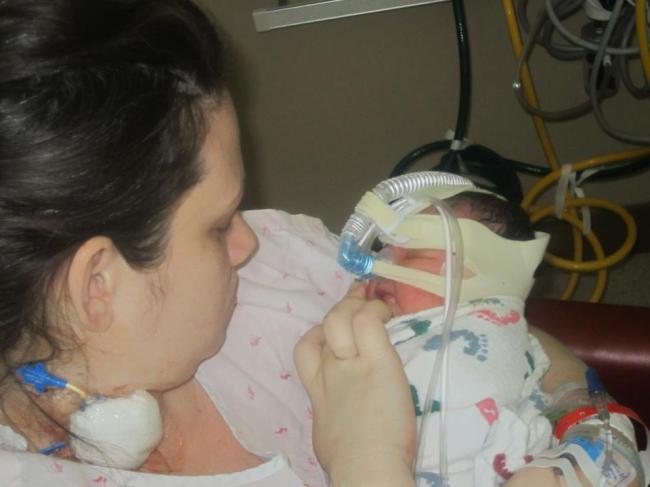
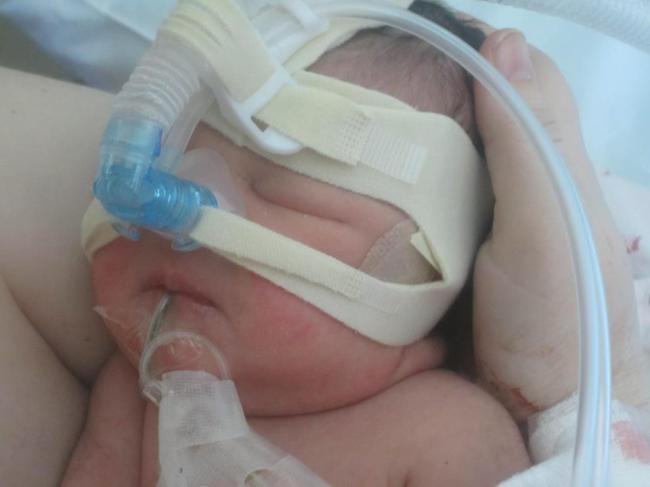
Later that morning I was moved to the maternity ward because I was recovering well. It was not easy to be there and see all the moms with their babies, while my baby was over in the NICU and separated from me. I pumped every 2 hours to try and get my milk to come in as soon as possible, although they weren’t allowing her to eat at this point. They saved what I pumped though, and would give it to her via the OG tube once the doctor allowed her to begin eating. At this point, she was receiving what she needed from the IV. Later that day I was given the happy news that she was being taken off the ventilator and moved to a CPAP, which was a step in the right direction. I was also told that I would be able to hold her once that happened. I pestered the nurses and NICU staff constantly, and as soon as I got the news that she was switched to the CPAP, they wheeled me back to the NICU so I could hold her. Oh, what a wonderful thing that was! I still couldn’t nurse her, but it was wonderful to have my baby in my arms and be able to have some skin-to-skin time. I even got to see her with her eyes open for a moment!
She still slept most of the time, though. I visited her every few hours, and pumped in between. I slept very little, but I was okay because all I cared about was devoting every waking second to getting my baby better. I was weak and exhausted, but I assumed it was because of the lack of sleep. Everyone kept telling me how pale I was, and I was having some breathing difficulties, but I was completely distracted by the baby’s needs. I was still struggling to manage the pain, but I was forcing myself to get up and walk and speed up my recovery for Annie’s sake.
At this point bad news seemed to come every time I got an update. Annie’s lungs were filled with fluid so her breathing was labored. They suspected pneumonia and ordered tests. Blood work came back showing an infection. It went from her being expected to be released from the NICU in 24 hours to being told she would probably be there for at least a month. She had done a little better and they were lowering her oxygen level, but then she regressed and they needed to increase her oxygen. They cultured mucous samples from her lungs because of the blood work indicating an infection. At one point they tried to get an IV in through her umbilical cord, but the IV broke off inside her. That happened while Tristan I were in the room with her. They kicked us out of the room and paged the neonatologist. They were just about to rush her into surgery when the doctor managed to get it out. It seemed like every time I turned around, I was being terrorized with more bad news.
On day three she was moved from the CPAP to a high flow nasal cannula. This was what I had been waiting for – I could finally nurse my baby! Up to that point she had been given what I pumped mixed with a little donor milk and fed through her OG tube (a tiny tube run down her mouth into her stomach). I was very happy that she took right to breastfeeding and we had no issues getting her to latch! She was weighed before and after each feed to see how much she got. My milk still wasn’t in yet, but she was getting colostrum. The would then supplement the rest if her feed with donor milk through the tube with was now fed down her nose and into her stomach. I nursed her every three hours on the dot. I would set an alarm on my cell phone and when it went off, I would head down the long hall from the maternity ward to the NICU. I would go through the cycle of washing my hands in the wash area, then head to her “pod” (which was what they called her little room). I would change her diaper, then nurse her, then put her back into the bed and head back to my room. Then I would pump so I could get my milk to come in. After that I would sleep for about an hour, then get up and do it again.
I was still so exhausted and pale. I was on oxygen now, and every time they tried to take me off my oxygen levels would drop. My doctor was concerned. She ordered some blood tests, and it seems that the blood I lost during surgery was not replenishing on its own, so she ordered a transfusion. I wasn’t exactly happy about that, but after I got it I became to feel so much better! My color began to return, and I started to feel better within hours. My pain was under control at this point, and my recovery was coming along. Annie was also beginning to do well, for which I was so grateful. They were able to rule out an infection. It seems the blood work they initially did was somehow tainted, and the mucus sample showed no infection. She was breathing a little better every day.
Then we had another setback. She developed jaundice and her bilirubin levels got too high. She had to be under the bill lights to get her levels down. We were told that as soon as she began to gain some weight and get her bilirubin levels stabilized, she could go home, but that she would have to be on home oxygen for an unknown amount of time.
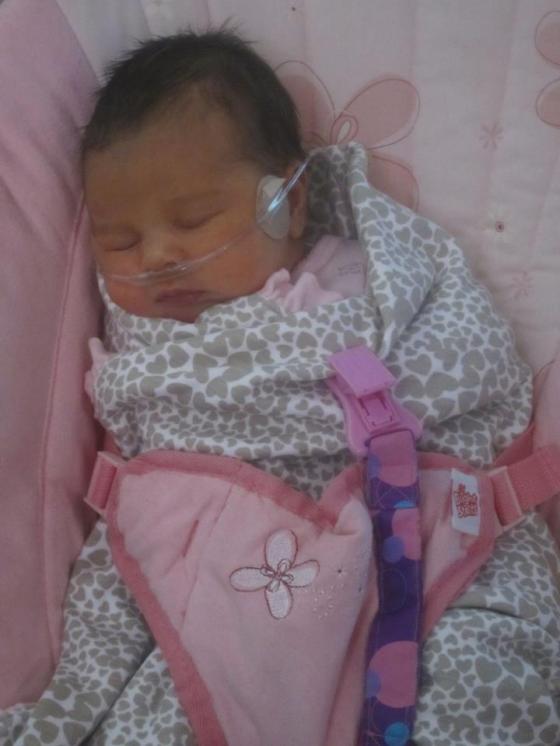
On day four my milk came in. I was thrilled! She no longer needed any supplementary donor milk, so the NG tube was removed. She was also moved to a low flow nasal cannula at this point, but her bilirubin was still too high. I continued the routine of nursing every three hours, always going back and forth between the NICU and my room in the mother/baby wing. My life revolved around that tiny little baby, and I was beginning to forget what like was like outside the NICU! I slept very little, but I welcomed the exhaustion. On day six I was discharged from the hospital. I packed up all my stuff and headed straight to Annie’s room. I was prepared to sleep in the little chair by her bed until she was also discharged from the hospital, but a miracle occurred! Over night she put on weight and her bilirubin numbers decreased. They told me that I could room-in with her in a special room that they had in the NICU for babies who were about to be released. That night was the first time that I was able to be with my baby all night long. I slept in the bed, and her little bassinet was right there by my side.
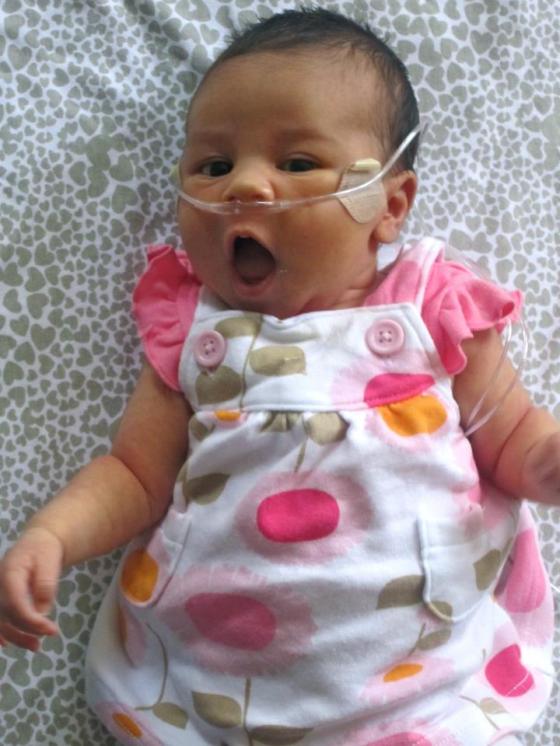
The next morning they did more blood work and weighed her again. She passed with flying colors, so we were given the okay to bring her home. How thankful I was!! It felt wonderful to finally be at home with all four of my children.
She was sent him on oxygen and we had to have a big tank in the house, plus little travel oxygen tanks for when we went out. It took some getting used to, but it was worth it to have her at home with us, and thankfully she only needed it for a month.
It took some time for me to come to terms with everything. Things were so hectic at the hospital that I never had the chance to process anything that happened. When I got home, I immediately began having nightmares about horrible things happening to my baby at the hospital, or bad things happening to me during surgery. That went on for weeks and weeks, and I struggled to sleep because of it. I would lay awake for hours, replaying everything that happened and remembering the fear of not knowing what was going to happen to my baby, and when I did sleep I was terrorized by nightmares. But, slowly, I began to move away from the pain. I am thankful that right aroud this time we got the news that we were going to be relocating because of my husband’s job, as it was able to consume my thoughts and help me emotionally recover from everything that happened during that week at the hospital. I am truly grateful for the care we received at the hospital. I’m thankful for the donor breastmilk that helped my baby before my milk came in, and for the surgery and blood transfusions that saved my life. I am thankful for God’s hand, that was so clearly there every step of the way.
It’s been nearly two years since Annie was born, and she is still every bit the miracle that she was then. She is happy, healthy, and she completes our family perfectly. I am also happy to report that she is still breastfeeding like a champ! Not a day goes by that I don’t give thanks to the Lord for this precious gift he’s given us.






No comments:
Post a Comment